Nursing
The Hingham Public School Nurses are essential members of the educational team. Our mission is to foster the growth, development and educational achievement of all students by promoting health and wellness, in a safe and supportive environment. We are committed to meeting the health needs of individual students and through collaboration with public and private agencies and health care providers, we advocate for students, their families and the school community.
Our Nurses
District Nurse Coordinator
Meredith Johnston, MEd, BA, RN
Hingham Middle School
Office: 781-741-4121
Hingham High School
Kristina McManus, MSN, RN, NCSN, CNOR, NE-BC
Hingham High School
781-741-1560 x2095
Kristine O’Keeffe, BSN, RN
Hingham High School
781-741-1560 x2095
kokeeffe@hinghamschools.org
Hingham Middle School
Jamie von Freymann, M.Ed, BSN, RN
Hingham Middle School
781-741-1550 x4047
jvonfreymann@hinghamschools.org
Samantha Landers, RN, BSN
Hingham Middle School
781-741-1550 x4047
East Elementary School
Callie Shanahan, BSN, RN, NCSN
East Elementary School
781-741-1570
cshanahan@hinghamschools.org
Foster Elementary School
Heidi Vigneau, MS, BSN, RN, NCSN
Foster Elementary School
781-741-1520
hvigneau@hinghamschools.org
Plymouth River Elementary School
Kristin Godfrey, RN, BSN
Plymouth River Elementary School
781-741-1530
South Elementary School
Carol Lincoln M.Ed, BS, RN, NCSN
South Elementary School
781-741-1540 x4214
clincoln@hinghamschools.org
Philosophy
The National Association of School Nurses defines school nursing as: “A specialized practice of professional nursing that advances the well-being, academic success, and lifelong achievement of students. To that end, school nurses facilitate positive student responses to normal development; promote health and safety; intervene with actual and potential health problems; provide case management services; and actively collaborate with others to build student and family capacity for adaptation, self management, self advocacy, and learning.”
Hingham Public School Nurses endorse the following beliefs developed by the American School Health Association and The National Association of School Nurses:
- Every child is entitled to educational opportunities that will allow him/her to reach full capacity as an individual and prepare him/her for responsibility as a citizen.
- Every child is entitled to a level of health which permits maximum utilization of educational opportunities.
- The school health program, through the components of health service, health education and concern for the environment, provides knowledge and understanding on which to base decisions for the promotion and protection of individual, family and community health.
- Parents have the basic responsibility for the health of their children; the school health program activities exist to assist parents in carrying out their responsibilities.
- The core roles that the school nurse fulfills to foster student health and educational success include; providing direct care to students, providing leadership for the provision of health services, providing/coordinating screening and referral for health conditions, promoting a healthy school environment, promoting/providing health education, serving in leadership roles for health policies and programs, being a liaison between school personnel, family, health care professionals, and the community.
Goals
- Reduce health-related barriers to learning and health related absenteeism thus improving student achievement
- Promote the health, safety, and wellness of all students and staff in the Hingham Public Schools
- Promote a positive, collaborative relationship with students, families, colleagues, and the community
- Promote best practices in school health services through professional development and resources.
Information, Documents & Resources
Asthma
Asthma is a chronic disease that affects your ability to breathe. Your airways, the tubes that carry air in and out of your lungs, become tight, swollen and produce mucus. The airways are also sensitive, and may react strongly to things that you are allergic to or find irritating. Symptoms of asthma are wheezing, coughing, chest tightness and trouble breathing. Asthma can cause symptoms ranging from minor wheezing to life-threatening asthma attacks. – MA Department of Public Health
School nurses help students with asthma stay in control and stay in school. If your child has asthma please contact your child’s school nurse for assistance. Keeping students with chronic health conditions in school is a health partnership between the parents/guardians, guidance counselors and school health services.
An Asthma Action Plan should be sent to your child’s school nurse at the start of each school year, upon a new diagnosis of asthma or with any changes to the action plan during the school year.
An inhaler may be kept in the nurse’s office, or students may carry their own inhalers during the school day (except in elementary school–inhalers will be with the nurse).
Please download the asthma action plan form below if needed.
Sources: www.aafa.org, www.mass.gov/asthma-prevention-and-control
Attendance Guidelines for Illness
When should I keep my child home from school?
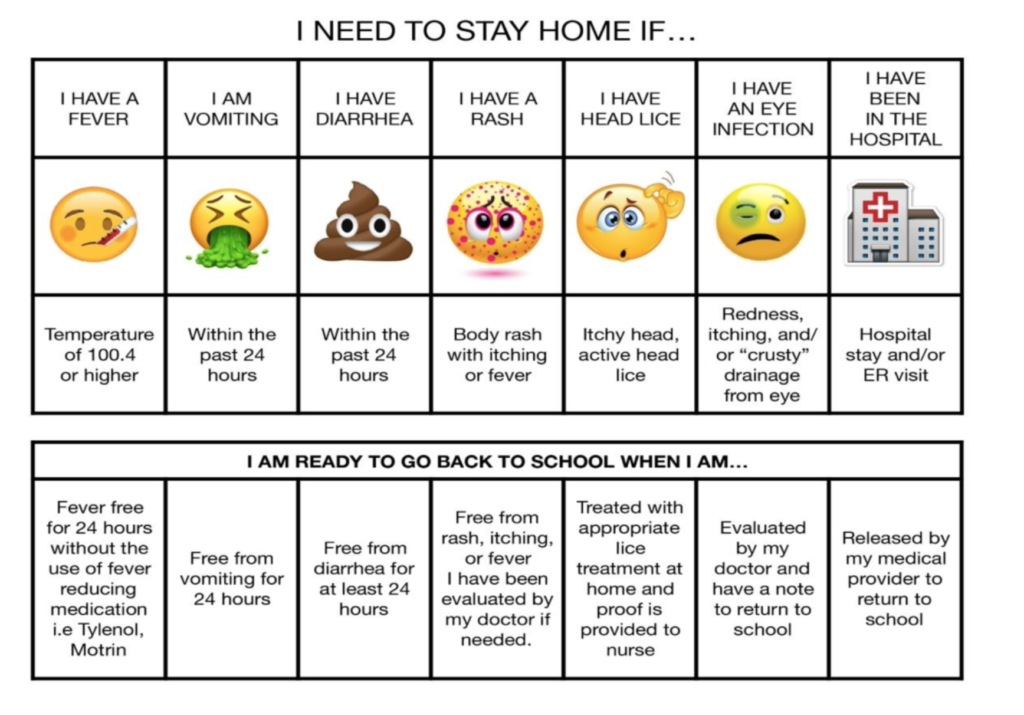
The Hingham Public School’s health policy, regarding school attendance and illness, asks that you please keep your child home from school if he/she….
- Has a fever of greater than or equal to 100.4 F within the past 24 hours. A student must be fever free for 24 hours without the use of a fever reducer medication such as ibuprofen (Motrin, Advil) or acetaminophen (Tylenol)
- Has vomiting or diarrhea within the past 24 hours
- Has been dismissed from school due to fever, vomiting, diarrhea or other communicable illness and may not return to school the next day
- Has an unexplained rash or draining skin sores (Provide health care provider’s note upon return to school)
- Is being treated for a contagious illness such as: Strep Throat, Impetigo, Pink Eye (Conjunctivitis) and must remain at home until on antibiotics for a full 24 hours (Provide health care provider’s note upon return to school)
- Has active infestation of head lice . Child should be checked by the school nurse before returning to school
- Has a cold in its active stages, with secretions and/or cough that can not be controlled.
If your child shows signs and symptoms of illness in school, it will be necessary for them to be picked up. Please keep all Emergency Contact Information up to date.
When you call or email that your child is absent due to illness or injury, please inform us of the nature of the illness or injury.
Thank you for your cooperation in helping to keep all of our students and staff healthy!
Communicable Illness Policy
In an effort to keep all of our students (and staff) healthy, we ask that you please read and follow our communicable illness/condition policy below:
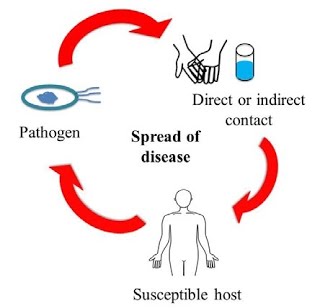
During the school year, communicable illnesses and/or conditions such as strep throat, mononucleosis, staph infections, seasonal flu (influenza), fifth disease, stomach viruses, as well as, pediculosis (head lice) may be prevalent. In order to reduce the spread of these illnesses or conditions in school, we are asking that you please observe your child carefully and frequently for any signs and symptoms. The most common symptoms for many of these illnesses/conditions are fever, cough, runny nose, sore throat, rash, vomiting, diarrhea. Head lice causes an itchy scalp.
If your child displays any of these signs and symptoms, please keep them home from school. By doing this, you will help prevent your child from having a difficult time with the illness during the school day, and it will prevent transmitting the illness to other children and staff. Please be aware that students must be fever-free (without fever reducing medications) and/or no vomiting or diarrhea for at least 24 hours before returning to school. A fever is defined as a temperature of 100.4F or higher.
A frequent examination of your child’s scalp is advised because unknown exposure to head lice, both in and out of school, may occur at any time. After being treated for head lice, your child must be checked by the school nurse before re-entering school.
All students returning to school after having a communicable illness must present a note from their health care provider stating the nature of the illness. They may not return to school without a certificate as prescribed by the Massachusetts Department of Public Health.
The following illnesses must have a doctor’s note in order to return to school:
- Strep Infection
- Impetigo
- Scarlet Fever
- Mononucleosis
- Mumps
- Measles
- German measles
- Whooping Cough
- Encephalitis
- Chicken Pox
If a child has other communicable illnesses such as conjunctivitis (pink eye) and influenza (flu), please inform and consult with the school nurse relative to the child’s return to school. If you have any questions, please feel free to contact your school nurse.
Thank you for your help in keeping all of our students (and staff) happy and healthy this school year!
Concussions
A concussion is a traumatic brain injury, caused by a blow or jolt to the head, that can temporarily or permanently impair a student’s physical abilities and change how the student thinks, acts and learns in school.
Physical symptoms that may occur are headache, nausea, light and noise sensitivity, fatigue, dizziness, blurred vision, changes in emotional state and short-term memory, and reduced concentration. Concussions may impact school performance with regards to organizational skills and completing assignments and tests.
It is important that a physician evaluates your child for any concussion symptoms and designs a plan of recovery with you as parents and the school. There are usually four stages of recovery:
| Red Stage | Students typically do not attend school (2-4 days). TV, reading, cell phone & computers are limited. |
| Orange Stage | School attendance is half days and activity continues to be limited. |
| Yellow Stage | School attendance is full day. Increasing homework and major test taking once a day. |
| Green Stage | School attendance is full-time and normal activities are resumed. |
The above stages will vary with each student, depending on the severity of symptoms.
Any student with a suspected concussion must see a physician and have a documented Concussion Plan of Recovery in place at school. A physician note is needed to return to school and to participate in sports. A physician note is also required to be excused from MCAS testing.
For more information on concussion and the treatment plan, please visit www.cdc.gov/concussion.
Below is the Head Injury Reporting Form for parents to fill out during sports season and the Post Head Injury Clearance form for your child’s physician to complete upon concussion clearance.
Click HERE to download the Head Injury Reporting Form to complete during sport season.
Click HERE to download Post Head Injury Clearance form for your child’s physician to complete upon concussion clearance.
Examinations & Screenings
State Mandated Health ScreeningsAccording to Massachusetts general laws, all students are required to have vision, hearing, body mass index (BMI) and postural screenings, andBrief Intervention and Referral to Treatment (SBIRT) at certain grade levels in school. Parents & Guardians may opt out of any screening. Please notify your child’s school nurse in writing if this is the case.
Students entering Kindergarten are required by Massachusetts General Law, Chapter 71 and Section 57, to have a pre-school vision screening which includes stereopsis. Please contact your child’s health care specialist for more information.
The schedule for health screenings is as follows:
Vision: Grade 1 through grade 5 and once in grade 6-8 and once in grade 10
If a student does not pass the vision screening, a referral letter recommending further evaluation by thier care provider or eye specialist, will be sent home. Please contact your child’s physician or health care provide promptly for an evaluation if you are notified that your child has not passed the vision screening. Early detection and correction may prevent problems in school performance and permanent vision loss. Optimal vision is essential in order for your child to acquire the knowledge and skills necessary to maximize their educational experience and success.
Hearing: Kindergarten through grade 3 and once in grade 6-8 and once in grade 10
Students who do not pass the initial hearing screening are rechecked at a later date, as a decrease in hearing may be related to cold symptoms or congestion. If a student does not pass the hearing screening a second time, a referral letter recommending further evaluation by their care provider will be sent home.
Please contact your child’s physician or health care provider promptly for an evaluation if you are notified that your child has not passed the hearing screening. Early detection and correction may prevent problems in school performance and permanent hearing loss. Optimal hearing is essential in order for your child to acquire the knowledge and skills necessary to maximize his/her educational experience and success.
BMI: Grades 1, 4, 7 & 10
Postural: Grades 5 through 9
SBIRT: Grades 7 & 9
SBIRT is an evidence-based screening to promote prevention and identify early risk for substance use in adolescents. Hingham High School (HHS) will screen all students in grade 9 during P.E. class, elective classes or study hall. Student screening sessions will be brief (approximately 5 minutes) and all confidential screenings will be conducted in private one-on-one sessions by the nurse. We will utilize the CRAFFT-II screening tool, which is the Department of Public Health (DPH) recommended substance tool. Please refer to www.masbirt.org for further information and resources.
Students who report that they are not using substances will have their healthy choices reinforced by the nurse. The nurse will provide brief feedback to any student who reports using substances or who is at risk for future substance use. Results of the screening are confidential and will not be included in your student’s school record, nor will the results be shared with parents or any school staff without written consent from the student. If the nurse feels there is a potential for your child to engage in risky behavior in the immediate future or identifies a risk to your child’s safety, they will be referred to the appropriate counseling staff for further evaluation. All students will receive educational material and a resource list at the time of the screening.
All screenings are performed in accordance with the Commonwealth of Massachusetts regulations. Students may also be screened at any time during the year at a teacher or parent’s request. If screening results indicate the need for follow-up care by a physician, parents/guardian will be notified in writing.
Health Notices & Advisories
Head Lice (Pediculosus)
Head lice are tiny, wingless insects that live close to the human scalp. They feed on human blood. When checking for head lice, you may see several forms: the nit, the nymph, and the adult louse. Nits are tiny, teardrop-shaped lice eggs that are often yellowish or white. Nits are attached to the hair shaft and often found around the nape of the neck or the ears. Nits can look similar to dandruff, but cannot be easily removed or brushed off. Nymphs, or baby lice, are small and grow to adult size in 1 to 2 weeks. Adult lice are the size of a sesame seed and appear tan to grayish white. (NASN)
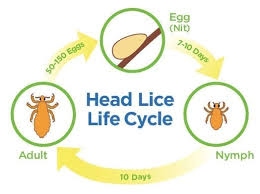
Head lice can be a nuisance but they have not been shown to spread disease. They are found worldwide and are most commonly found in school aged children and in the household members of infested children. Head lice move by crawling; they cannot hop or fly. Head lice are spread by direct contact with the hair of an infested person. Anyone who comes in head-to-head contact with someone who already has head lice is at greatest risk. Spread by clothing (such as hats, scarves and coats) or other personal items (such as combs, brushes or towels) used by an infested person is uncommon. Personal hygiene or cleanliness in the home or school has nothing to do with getting head lice. (CDC)
Signs and symptoms of infestation include:
• Tickling feeling on the scalp or in the hair
• Itching (caused by the bites of the louse)
• Irritability and difficulty sleeping (lice are more active in the dark) • Sores on the head (caused by scratching, which can sometimes become infected)
Finding a live nymph or adult louse on the scalp or in the hair is an indication of an active infestation. They are most commonly found behind the ears and near the neckline at the back of the head. (NASN)
Hingham Public Schools – Guidelines for Head Lice
1. Children will be sent home from school for treatment if a case of head lice infestation has been found. An active infestation is determined if the school nurse identifies live lice and/or many nits within one-quarter inch of the child’s scalp. (CDC)
2. Efforts will be made by the school nurse to check other students in the school known to be in close contact with the infested student.
Classroom-wide student head checks will no longer take place. (NASN)
3. After being treated at home, students must be checked by the school nurse before returning to class. The nurse will make a determination as to whether the child will be allowed to remain in school.
4. Parents will be encouraged to check their child’s head periodically throughout the school year.
5. Informational fact sheet will be made available on Hingham Public School Web-site.
6. A head lice notification letter will be sent home to specific grade levels or classrooms that have students with active head lice.For more information about head lice, please visit:
MRSA
Questions and Answers About Methicillin-resistant Staphylococcus aureus (MRSA)
MRSA is sometimes said as a single word, “mersa,” or by saying all four letters, “M-R-S-A”
What is MRSA?
MRSA is a kind of bacteria that is resistant to some kinds of antibiotics. To understand MRSA it is helpful to learn about Staphylococcus aureus bacteria, often called “staph,” because MRSA is a kind of staph.
What are staph?
Staph are bacteria commonly carried on the skin or in the nose of healthy people. About 25-30% of the U.S. population carry staph on their bodies at any time.
Do staph always make people sick?
No. Many people carry staph in their nose or on their skin for a period of time and do not know they are carrying them. They do not have skin infections. They do not have any other signs or symptoms of illness. This is called “colonization.”
Sometimes, though, staph can cause an infection, especially pimples, boils and other problems with the skin. These infections often contain pus, and may feel itchy and warm. Occasionally, staph cause more serious infections.
How are staph spread?
Staph are spread by direct skin-to-skin contact, such as shaking hands, wrestling, or other direct contact with the skin of another person. Staph are also spread by contact with items that have been touched by people with staph, like towels shared after bathing and drying off, or shared athletic equipment in the gym or on the field.
Staph infections start when staph get into a cut, scrape or other break in the skin. People who have skin infections—painful, swollen pimples, boils, and rashes, for example—should be very careful to avoid spreading their infection to others.
Is MRSA different from other staph?
Yes. MRSA is different from other staph because it cannot be treated with some antibiotics. When antibiotics are needed to treat a MRSA infection, the right antibiotic must be used. If the right antibiotic is not used, the treatment may not work.
MRSA is just like other staph in almost every other way:
- MRSA can be carried on the skin or in the nose of healthy people, and usually not cause an infection or make them sick.
- It can cause minor skin infections that go away without any special medical treatment.
- It is spread the same way as other staph.
- The symptoms are the same as other staph infections.
What are the symptoms of an infection caused by staph?
Pimples, rashes, pus-filled boils, especially when warm, painful, red or swollen, can mean that you have a staph or MRSA skin infection.
Occasionally, staph can also cause more serious problems such as surgical wound infections, bloodstream infections and pneumonia. The symptoms could include high fever, swelling, heat and pain around a wound, headache, fatigue and others.
What should I do if I think I have a staph skin infection?
Keep the area clean and dry. See your doctor, especially if the infection is large, painful, warm to the touch, or does not heal by itself.
How will my doctor know if I have a MRSA infection?
The only way to tell the difference between MRSA and other staph infections is with lab tests. Lab tests will also help your doctor decide which antibiotic should be used for treatment, if antibiotic treatment is necessary.
Your doctor will usually take a sample on a swab (like a Q-tip) from the infected area. The
sample will be sent to a laboratory to see if the infection is caused by staph. Blood and other
body fluids can also be tested for staph.
How are MRSA infections treated?
Most MRSA skin infections are treated by good wound and skin care: keeping the area clean and dry, washing your hands after caring for the area, carefully disposing of any bandages, and allowing your body to heal.
Sometimes treatment requires the use of antibiotics. Lab tests help your doctor decide which antibiotic should be used for treatment, if antibiotic treatment is necessary. If antibiotics are prescribed, it is important to use the medication as directed unless your doctor tells you to stop. If the infection has not improved within a few days after seeing your doctor, contact your doctor again.
How can I prevent a staph infection?
- Regular handwashing is the best way to prevent getting and spreading staph, including MRSA. Keep your hands clean by washing them frequently with soap and warm water or use an alcohol-based hand sanitizer, especially after direct contact with another person’s skin.
- Keep cuts and scrapes clean and covered with a bandage until they have healed.
- Avoid contact with other people’s wounds or bandages.
- Avoid sharing personal items such as towels, washcloths, toothbrushes and razors. Sharing these items may transfer staph from one person to another.
- Keep your skin healthy, and avoid getting dry, cracked skin, especially during the winter. Healthy skin helps to keep the staph on the surface of your skin from causing an infection underneath your skin.
- Contact your doctor if you have a skin infection that does not improve.
For more information about MRSA, visit the MDPH website
Source: MA Department of Public Health
Sun Protection
Ticks & Lyme Disease
- Always make sure to check yourself daily for ticks.
- Wear appropriate clothing when in wooded areas making sure to wear long sleeves and long pants.
- If you obtain a tick bite contact your physician for more information. The Centers for Disease Control, (CDC) has some helpful tick information. The information includes tips for preventing tick bites, types of ticks with illustrations and tick carrying diseases and more.

Vaping

Vaping is the inhalation of “vapor” created by an electronic cigarette (e-cigarette) or other vaping device.
E-cigarettes are electronic smoking devices. They have cartridges filled with a liquid that usually contains nicotine, flavorings, and chemicals. It also can contain THC, the chemical in marijuana that makes the user feel “high.” When the liquid is heated, it forms a vapor, which the person inhales. That’s why e-cigarette use is referred to as “vaping.”
What Are the Health Effects of Vaping?
While we don’t know the full extent of long-term effects of vaping, health experts have already reported serious lung disease, lung damage, and even death related to vaping.
Vaping puts nicotine into the body. Nicotine is highly addictive, and can have negative impact on brain development in children and teens. Memory, concentration, learning, self-control, attention, and mood can all be affected. Vaping can also increase the risk of addiction to other substances.
There are many different kinds of vaping devices. Common terms include JUULs, e-cigarettes, e-cigs, smokeless cigarettes, vaporizers, vapes, vape pens, vapor pens, e-hookah and hookah pens. They come in different shapes and sizes. One popular device, the Juul, looks like a flash drive. It makes less smoke than other e-cigarettes, so some teens use them to vape at home and in school. One Juul pod contains the same amount of nicotine as a full pack of cigarettes.
Vaping Liquid:
The liquid used to vape most commonly contains three ingredients: propylene glycol and/or glycerin, chemicals for flavoring and nicotine. Some vape pods can also contain THC, the chemical in marijuana that makes the user feel “high.” Vaping doesn’t produce a lot of “smoke” and often doesn’t produce a smell.
Do I Have to Vape Every Day to Get Addicted?
No. Even if you don’t vape every day, you can still get addicted. Nicotine is a highly addictive substance, and binds to the reward receptors in the brain, similar to alcohol, heroin, and other substances of abuse. The adolescent brain is particularly sensitive to these substances, as it is undergoing massive growth and development during this time.
Nicotine enters the brain approximately 10 seconds after inhaled and causes a “feel good” reaction (the brain’s reward pathway). The feeling is short lived, however, because nicotine leaves the body relatively quickly. The brain then begins to crave the feeling produced by the nicotine.
What About E-cigarettes That Don’t Have Nicotine?
ALL Juul pods contain nicotine, as does most vape liquid. ALL vape liquid contains chemicals that can cause lung irritation and damage.
VIDEO: Vaping cost one teen his health and dreams.
How to Quit:

Additional Resources from the CDC:
- E-cigarettes and Youth: What Parents Need to Know pdf icon[PDF – 1 MB]
- Get the facts about electronic cigarettes, their health effects and the risks of using e-cigarettes
- What’s the Bottom Line About Electronic Cigarettes?
- What’s the Bottom Line on the Risks of E-cigarettes for Kids, Teens, and Young Adults?
- Marijuana and Public Health
West Nile Virus & EEE

West Nile Virus and Eastern Equine Encephalitis (EEE) are diseases caused by a virus. The virus is spread to humans through the bite of an infected mosquito. Mosquitoes become infected when they bite infected birds.Most people do not have symptoms when infected with West Nile Virus. Encephalitis, inflammation and swelling of the brain, is the most dangerous complication
The symptoms of EEE include: fever, stiff neck, headache and lack of energy. These symptoms show up 3-10 days after a bite from an infected mosquito.
There is no treatment for EEE.
PREVENTION & PROTECTION FROM EEE IS THE KEY!
Here are some things you can do to reduce your chances of being bitten:
- Avoid outdoor activities between dusk and dawn. This is when mosquitoes are most active.
- Wear long pants, long-sleeve shirt and socks while outdoors. This will help keep mosquitoes away from your skin.
- Keep mosquitoes out of your house by repairing any holes in your screens and make sure screens are attached tightly to all doors and windows.
- Remove areas of standing water around your home.
- Using a mosquito repellent is a family choice. For further information on choosing and using repellents safely, see MDPH Mosquito Repellent Fact Sheet on mass.gov/dph
- For more information on West Nile Virus & EEE, The Massachusetts Department of Public Health (MDPH) has a web-site on Mosquito-borne Diseases at www.mass.gov/dph.
- You may also contact your local board of health (listed in the telephone directory under “government”).
- You may also call MDPH toll-free at (888) 658-2850.
Mosquito control in your city or town: Mosquito control in Massachusetts is conducted through nine mosquito control districts. The State Reclamation and Mosquito Control Board (SRMCB) oversees all nine districts. Contact information for each district can be found online at mass.gov/dph. You may also contact the SRMCB within the Massachusetts Department of Agricultural Resources at 617-626-1700 or your local board of health.

District Forms
- Allergy Action Plan Form
- Immunization Exemption Form
- Medication Form – Parent
- Medication Order Form – Prescriber
- Medication Self-Administration Form (Day Field Trips)
- Medication Self-Administration Form (Overnight Trips)
- Student Health Emergency Form
- Asthma Action Plan Form
- In-Season Report of Head Injury Form
- Post-Head Injury Clearance Form